Post-accident dentistry, often handled by emergency and restorative dentists, focuses on
repairing, replacing, and stabilizing teeth and jaw structures damaged by traumatic incidents such as falls, accidents, or sports injuries. Treatment aims to provide immediate pain relief, prevent infection, and restore the functionality and aesthetics of the patient’s smile.
Common Post-Accident Dentistry Treatments
- Tooth Replacements (Missing Teeth):
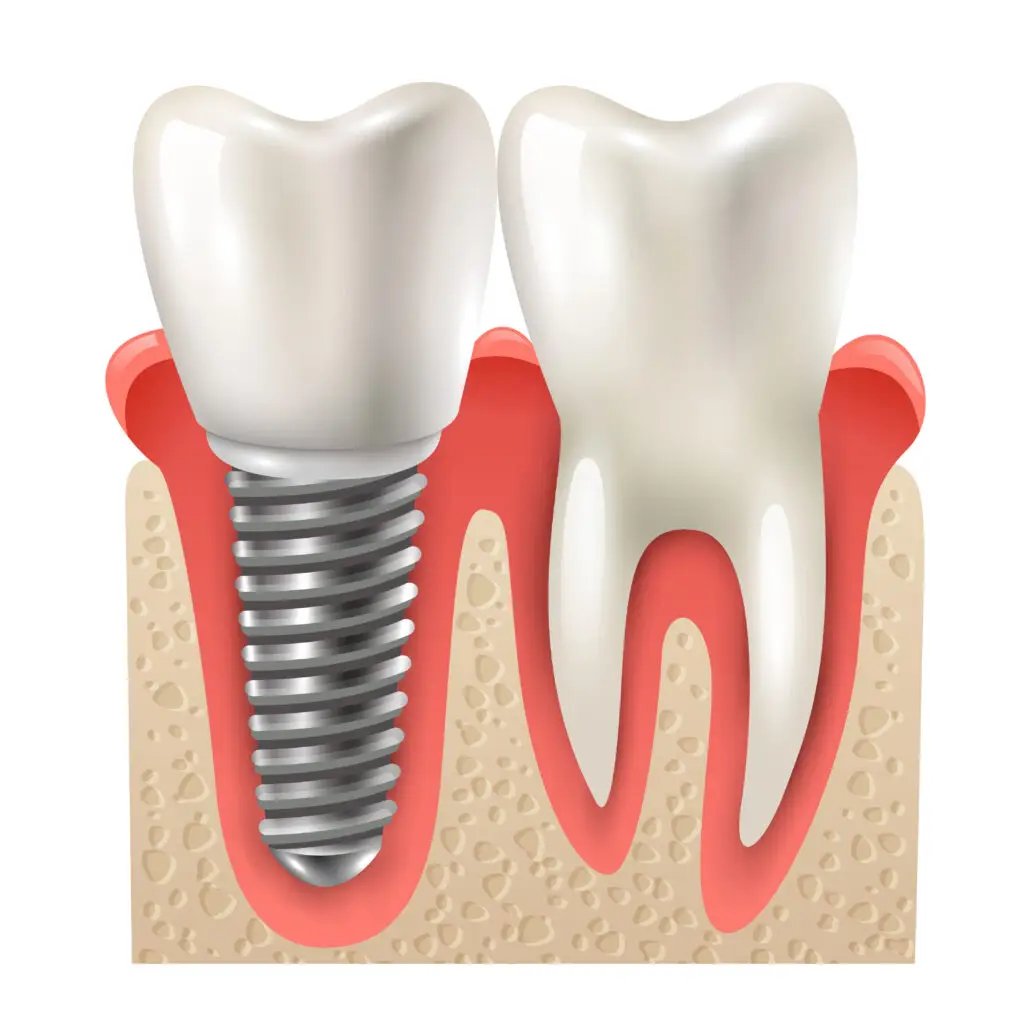
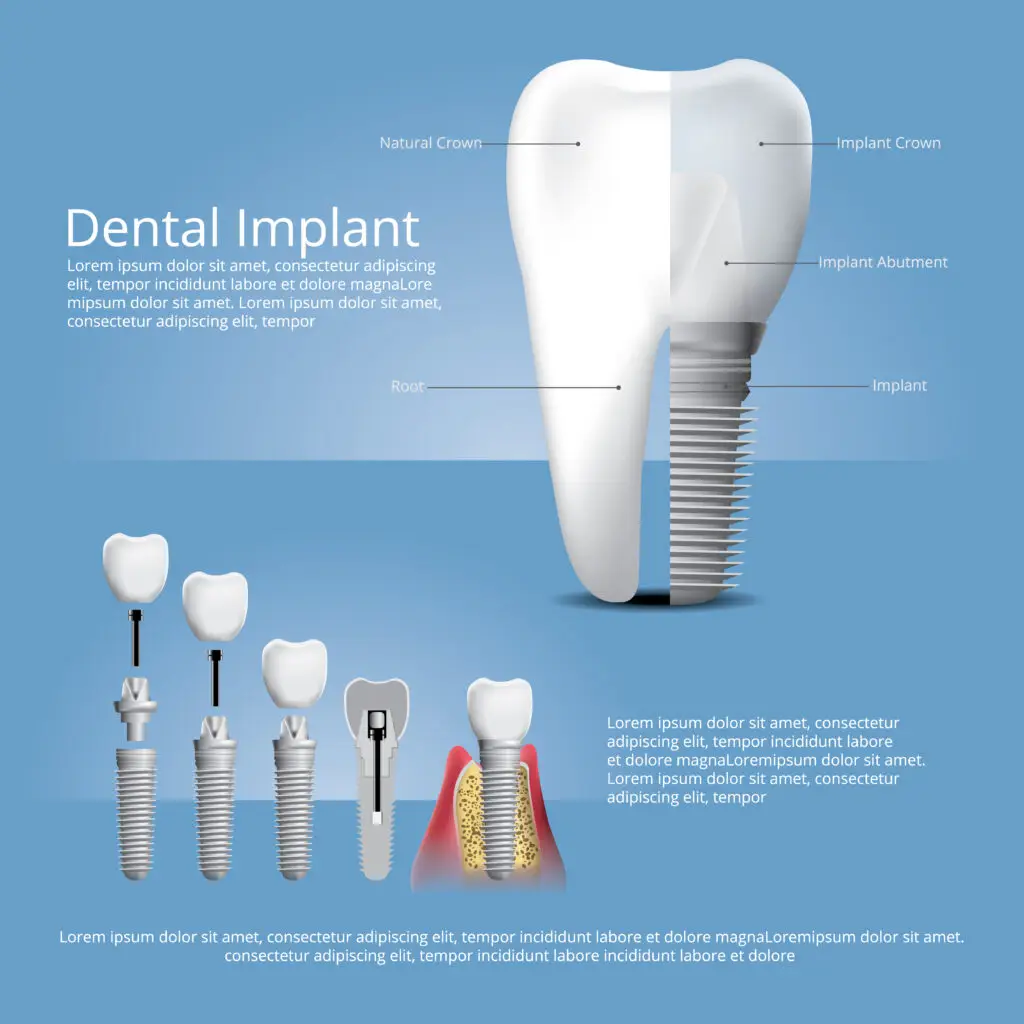
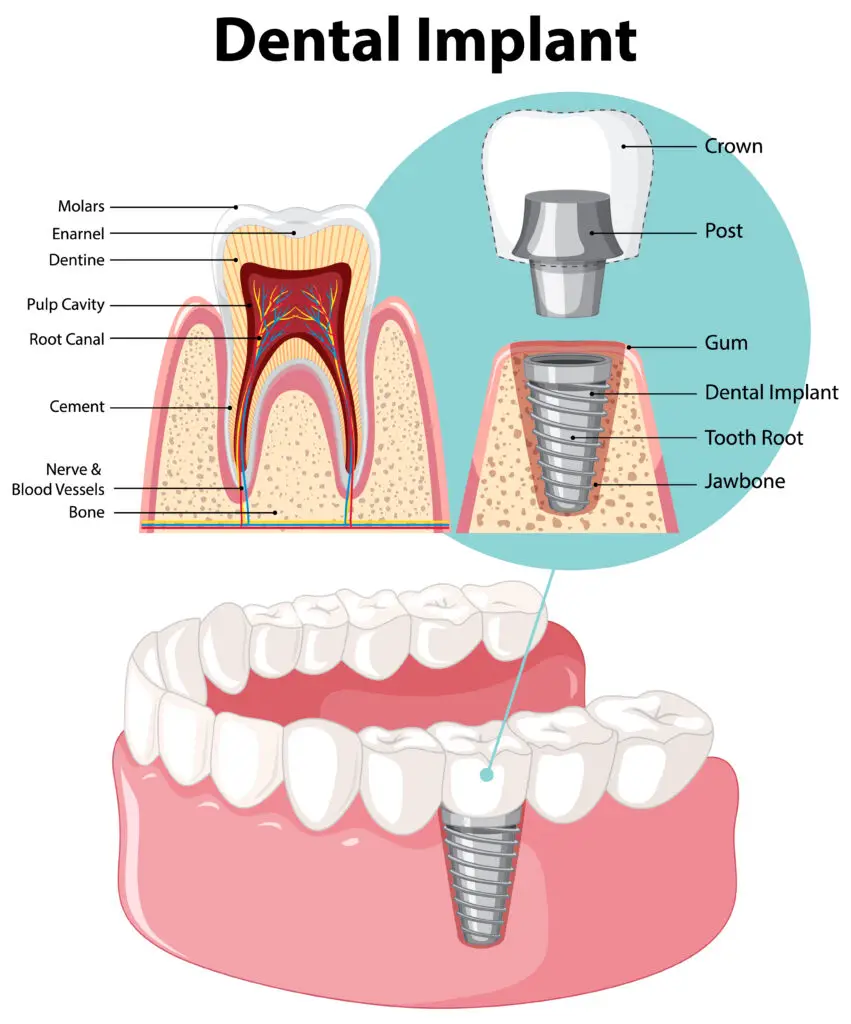
- Dental Implants: Often the preferred long-term solution, a titanium post is placed in the jawbone to serve as a new root, topped with a crown.
- Dental Bridges: Used to fill gaps by anchoring a false tooth to adjacent teeth.
- Partial or Complete Dentures: Removable alternatives depending on the severity of the tooth loss.
- Damaged Tooth Repair (Broken/Cracked/Chipped):
- Dental Bonding: Tooth-colored resin is used to repair minor chips or cracks, typically in one visit.
- Dental Crowns: Covers a fractured or severely damaged tooth to protect it and restore its shape and strength.
- Root Canals (Endodontics): Necessary if the accident damaged the tooth’s pulp (nerve) or resulted in an infection.
- Stabilization and Realignment (Loose/Shifted Teeth):
- Splinting: A flexible wire or composite is used to attach a loosened tooth to its neighbors, stabilizing it while the underlying tissues heal.
- Replantation: If a tooth is completely knocked out (avulsion), it can sometimes be reinserted into the socket within a “golden hour” of the injury, followed by splinting.
- Periodontal (Gum) and Soft Tissue Care:
- Gum Grafting/Contouring: Treats damaged gum tissue to ensure proper support for the teeth.
- Suturing: Repairs cuts or lacerations in the mouth, tongue, or gums.
- Preventive and Diagnostic Care:
- Digital Scans/X-rays: Essential for diagnosing hidden damage, such as root fractures, that are not visible to the naked eye.
- Antibiotic Treatment: Used to reduce the risk of infection following trauma.
- Temporomandibular Joint (TMJ) Management: Addressing jaw injuries that cause pain or “lockjaw”.